Just like our gut, our mouth is home to a microbiome – a living community of bacteria, viruses, and fungi. These microbes are not only necessary to maintain the health of our teeth and gums but also critical in maintaining overall health.
When the balance between the beneficial and harmful bacteria in our oral microbiome is tipped in the wrong direction (known as dysbiosis), the buildup of harmful bacteria can lead to a variety of oral diseases and conditions including cavities, gum disease, and halitosis (bad breath).
Our mouth is one of the primary entry points to our body and unsurprisingly, what happens in the mouth, doesn’t stay in the mouth. Increasingly, research has shown that certain oral bacteria and poor oral health are associated with a number of chronic systemic conditions including diabetes, Alzheimer’s, cardiovascular disease, cancer, and adverse pregnancy outcomes [*].
I’ve talked a lot about the importance of gut health and microbiome testing, but we’ve never had the ability to look at our oral microbiome – until now. Bristle has created the world’s first at-home oral microbiome test to help you measure, understand, and improve your oral health with personalized recommendations and coaching.
Here’s a closer look at how the oral microbiome is connected to our body and ways to hack your microbiome for optimal health, including testing with Bristle.
What is the Oral Microbiome?
Our mouths harbour the second-largest and diverse microbial community with trillions of living microbes. More than 700 unique species of bacteria have been found in the oral cavity with an average of over 100 species per person [*] [*].
These microorganisms are found throughout our mouth – inside of our cheeks, on our tongue, teeth, and every crevice in between. They can be found as free-swimming (planktonic) cells or connected together in a biofilm, a complex structure of microbes attached to surfaces.
Some of these microbes are beneficial (commensal) and critical to maintaining health and wellness, while others are harmful (pathogenic) and can directly cause disease.
Your Beneficial Bacteria
Feeding the beneficial bacteria in your mouth is vital for keeping your body functioning at peak levels.
Food digestion starts in your mouth where certain bacteria metabolize the food you eat. Normally, healthy microbes thrive and grow into niches, helping to prevent pathogenic microbes from invading and causing disease. These same bacteria also help stimulate saliva production. Saliva covers our teeth, acting as a protective barrier against harmful bacteria and washing away excess food particles. It also contains minerals essential to maintaining and restoring the integrity of our teeth through a process called remineralization.
Other oral bacteria provide health benefits beyond our mouths. For example, certain species help promote metabolic and cardiovascular regulation, and improve cognitive function [*]. These bacteria perform the critical process of reducing nitrate to nitric oxide, a powerful vasodilator molecule that regulates blood pressure. You can reap these benefits by eating foods high in nitrate like beets and leafy greens including kale, arugula, and spinach.
Maintaining balance in our oral microbiome is critical to good oral health. It is important to understand the current state of our oral microbiome and how the choices we make can affect it. For example, products including antibiotics and alcohol-based mouthwashes – used in the wrong context – can potentially cause harm by eradicating commensal bacteria alongside pathogenic species. Failing to re-populate our mouths with commensal species provides opportunities for pathogenic bacteria to thrive.
What Causes Cavities, Gum Disease, and Bad Breath?
Cavities and periodontal (gum) disease are two of the most prevalent diseases on the planet yet both are largely preventable. When your oral microbiome is out of balance, the pathogenic bacteria thrive and start wreaking havoc.
Cavities
Over 90% of adults 20 to 64 have had a dental cavity in a permanent tooth and over 25% have untreated tooth decay [*].
Bacteria form a biofilm on our tooth surfaces, also known as dental plaque. Most of the time, healthy plaque coats the tooth surface, and doesn’t cause disease. However, in some people, this plaque harbors acidogenic bacterial species, like Streptococcus mutans, which can convert sugar from drinks and foods we consume into acid. This acid eats away at the enamel, and eventually leads to cavities.
Risk factors for cavities include diet, poor oral health habits, dry mouth, smoking, diabetes, and acid reflux. Some studies have demonstrated that the bacteria that cause cavities are transmissible. Children of mothers with active tooth decay are therefore at increased risk of cavities [*], [*].
Periodontal (Gum) Disease
Half of US adults have some form of gum disease, which is irreversible in its later stages.
Periodontal pathogens like Porphyromonas gingivalis and Fusobacterium nucleatum accumulate around the gum line, releasing toxins that cause inflammation and damage to the surrounding gum tissue. Eventually, the bacteria deepen the pockets between your gums and teeth where more pathogens can grow. This process compounds as the pockets deepen, and the surrounding tissue and bones become irreparably damaged causing bone and tooth loss.
While gum disease can progress without visible symptoms, warning signs include receding or bleeding gums, loose teeth, bad breath, and redness or swelling of the gums.
Risk factors include inadequate nutrition, smoking or chewing tobacco, hormonal changes such as those related to pregnancy or menopause, diabetes, immunosuppression, and poor oral hygiene.
Halitosis (Bad Breath)
Over 50% of people experience halitosis or bad breath regularly. It can be embarrassing, cause stress in work interactions, and impact our social lives. It’s also often a reflection of other health issues.
90% of halitosis cases originate in the mouth [*]. Bacterial species such as Solobacterium moorei and Prevotella intermedia break down proteins in foods we eat and release volatile sulfur compounds (VSCs) as byproducts. VSCs are just one of the compounds responsible for the foul odor that comes from the mouth. A higher abundance of these oral bacteria is directly associated with the amount of VSCs produced, and accordingly how bad your breath smells [*]. Other anaerobic species are also able to create VSCs through anaerobic fermentation.
Oral bacteria also produce dozens of other foul smelling compounds that can contribute to halitosis [*]. Putrescine, cadaverine, and other volatile aromatic compounds are foul smelling bacterial byproducts created by specific communities of oral bacteria [*] [*]. Propionic and butyric acid smell distinctly like body odor and vomit, resulting from fermentation by specific oral bacteria.
Addressing the root cause of bad breath means reducing the abundance of these bacteria. While gum, mints, or mouthwash might provide temporary relief, they are only masking the byproducts of the underlying bacteria.
Your Mouth is the Gateway to Your Body
Your oral microbiome plays an essential role in your overall health. It is the first line of defense against foreign pathogens and at the same time, an entry point for severe infections. Pathogenic bacteria that cause inflammation in your mouth can lead to inflammation in the rest of your body. Inflamed gums cut more easily, allowing bacteria to enter your bloodstream and travel throughout your body.
Through a proper oral hygiene routine, diet, and lifestyle, you can maintain a healthy oral microbiome, reduce your risk for chronic diseases, and increase your longevity. You can’t be healthy without a healthy mouth.
Tips for a Healthier Oral Microbiome
The key is to boost the good bacteria and get rid of the bad ones. To upgrade your oral health, follow these steps:
- Brush and floss regularly. One lesser known tip is not to brush your teeth right after a meal. Foods and drinks can cause your mouth to become acidic and you damage your enamel if you brush right after, so wait at least 30 minutes.
- Use a tongue scraper. Bacteria (especially those that cause bad breath) love to live on your tongue, so use a scraper to disrupt the biofilm.
- Stay away from alcohol-based mouthwash. It kills off the good guys along with the bad guys, and is associated with high blood pressure.
- Take an oral probiotic. Probiotics like S. salivarius K12 and M18 have shown to help with halitosis.
- Stay hydrated. Water helps increase saliva production and wash away food particles that bacteria can feed on.
- Have mints or chew gum with xylitol after meals. Xylitol is a natural sugar alcohol that inhibits the fermentation process of bacteria that cause tooth decay and cavities. It can also stimulate saliva production, which is particularly helpful for dry mouth.
- Avoid refined carbs, sugar, acidic foods and drinks. Cavity-causing bacteria feed off sugar and release acid as a byproduct, destroying your enamel. These bacteria thrive in an acidic environment. If you do consume these foods and drinks, the key is to do it over a short period of time and drink water in between and after to minimize the acidity of your mouth.
- Feed the good bacteria. High-fiber vegetables and fruits, high pH alkalizing vegetables, and foods with high levels of arginine or vitamin K2 can help promote better oral health by remineralizing teeth, neutralizing acid, and reducing plaque buildup. Nitrate can also help boost bacteria that create nitric oxide, and may reduce blood pressure.
Biohack Your Mouth with Bristle
A one-size-fits-all approach almost never works when it comes to medicine because everyone is biologically different. The same principle applies to our mouths and oral health.
Our oral microbiome determines our risk for oral diseases and plays a fundamental role in our overall health, but everyone’s oral microbiome is unique. The same lifestyle, hygiene, and diet factors can impact two individuals very differently.
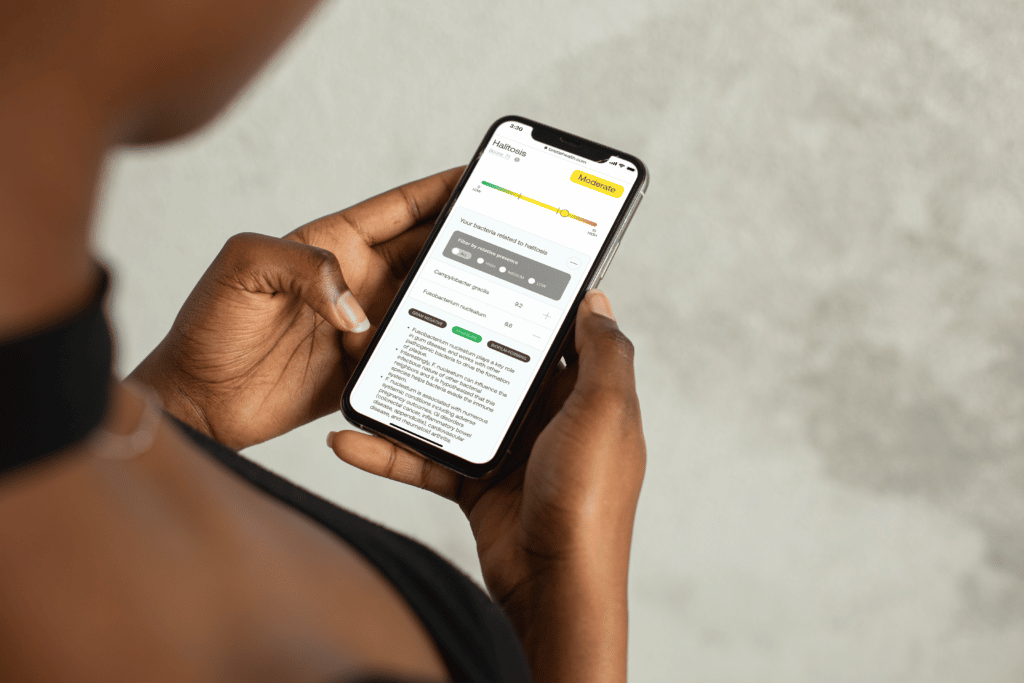
With Bristle, you can analyze your oral microbiome, see how it’s impacting your health, take steps to improve, and then quantifiably track your progress. Their at-home oral microbiome test measures every unique bacterial species (usually 100+ species) in your saliva, both beneficial and pathogenic, providing data on your oral health risks. No stool sample required, just a little spit in a tube!
The results include scores for tooth decay, gum inflammation, halitosis, gut inflammation, and beneficial bacteria. Each score has the contributing bacterial species detected in your microbiome, their levels, and information on their function in the mouth and associations with our health. You also get the full breakdown of all detected species and can see how you stack up against people diagnosed with oral disease.
Based on your test results, you’ll receive hygiene, diet, and oral care recommendations, including specific ingredients in oral care products that have shown efficacy in balancing the oral microbiome based on scientific research. You also receive 1:1 coaching with one of their oral hygiene specialists to review your results and work on a personalized action plan.
Bristle helps you get a snapshot of where you are at today and provides recommendations tailored to you to improve your oral microbiome. You can incorporate diet, lifestyle, and hygiene changes and then test regularly to monitor progress to your scores and changes in your oral microbiome. Start testing your saliva with Bristle and use the code DAVE15 for 15% off.
The cornerstone of any good biohacking regimen is quantification – tracking what we do and its measurable impact. We now have the ability to do that with our oral health and microbiome.